Methenamine decomposes at an acidic pH to form formaldehyde and ammonia, both of which are bactericidal. 
Patients with infective struvite stones are generally started on urinary acidification with vitamin C, 1 g daily, and methenamine, 1 g twice daily, for ≥ 6 months, if clinically indicated. Postoperative care should include a complete metabolic work-up with 24-hour urine collection to address any metabolic defects and reimaging in 6 months. As many as 80% of patients implicated the postoperative ureteral stent as the worst part of their operation, which is why we advocate a tubeless disposition upon discharge with complete stone clearance. 
We rarely leave a double J ureteral stent after PCNL, as we have demonstrated a significantly better quality of life using a temporary nephrostomy tube that is removed before discharge compared with a stent left in place for over a week. Patients who are completely stone free have all tubes removed prior to their discharge. Complete stone clearance after PCNL for staghorn calculi approaches 85% in the literature, and is higher at NYU Langone Medical Center. We obtain a CT scan after every PCNL to ensure stone clearance and assess need for a second-stage operation. The re-entry NUC allows tamponade of the tract for 24 hours, which substantially lessens the risk of tract bleeding. Many PCNLs for staghorn calculi are planned as staged operations with a second look through the original established nephrostomy tract. A stone culture is sent because the discordance rate between the intraoperative stone culture and urine culture organisms has been reported in upwards of 50% of cases. Antegrade ureteroscopy is performed at the conclusion of every case to ensure the absence of obstructing ureteral fragments. The goal is to maximize removal of the stone burden before visualization becomes hampered by bleeding or angle torque, for example. Sometimes, a second or even access tract is needed to facilitate complete stone clearance. The disadvantage with upper pole access is the risk of hydrothorax associated with supra-12th or 11th rib puncture in 10% and 30% of cases, respectively. The midpole calyces can usually be assessed from the upper pole, as well. Access into the posterior upper pole calyx is preferred as this vantage point provides a more favorable angle to visualize the renal pelvis, ureteropelvic junction, proximal ureter, and lower pole calyces. This allows unfettered entry into any calyx for optimal visualization and stone removal. Shockwave lithotripsy is a poor modality to treat staghorn calculi and should be avoided.Īt NYU Langone Medical Center (New York, NY), we are able to obtain percutaneous access directly into the kidney without the assistance of interventional radiology. American Urological Association guidelines for the surgical management of stones emphasize PCNL as first-line treatment. Failure to completely eradicate the struvite stone virtually ensures the regrowth of the stone. The primary goal of treatment is to completely remove the stone, preserve renal function, eradicate infections, and relieve obstruction. 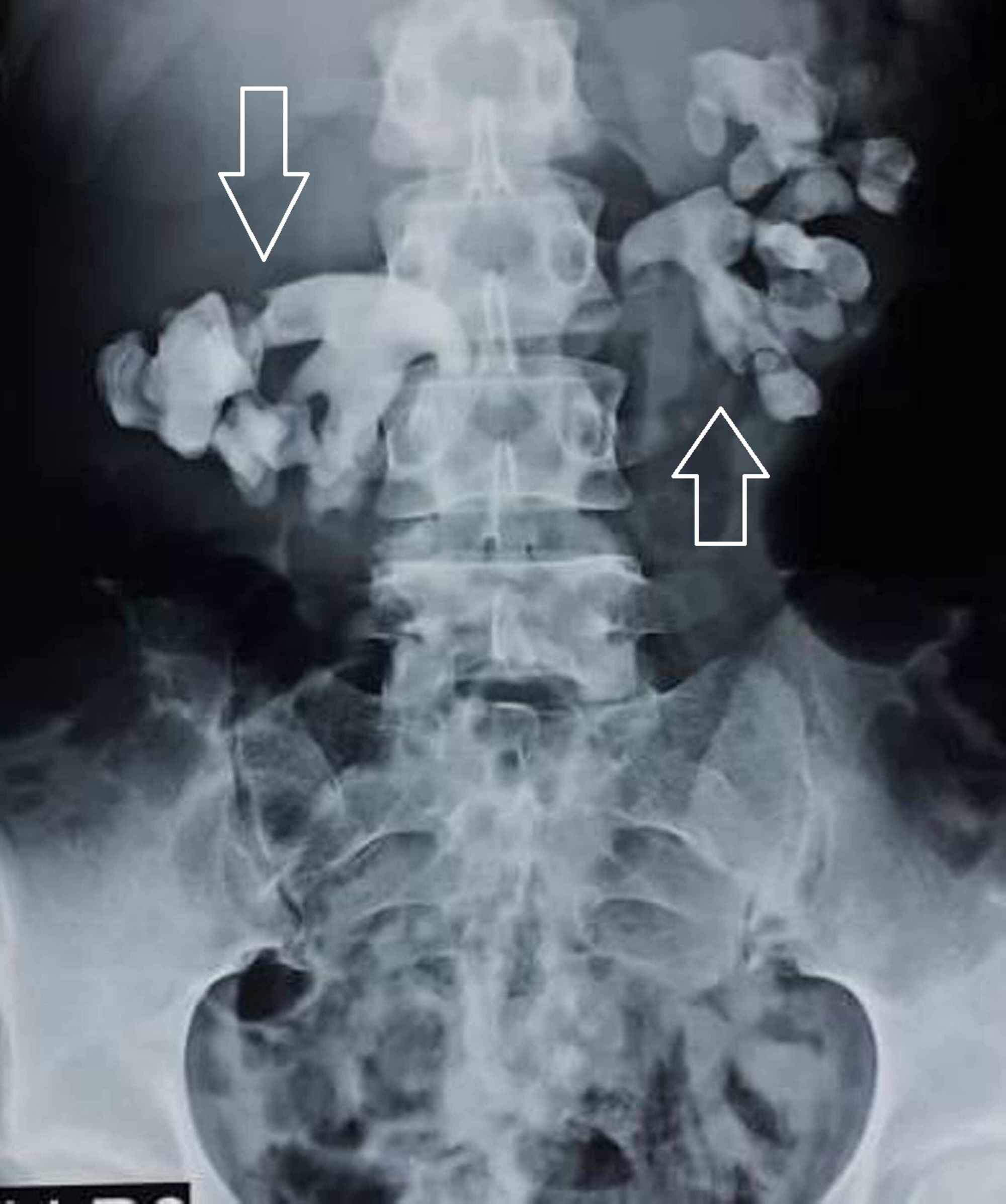
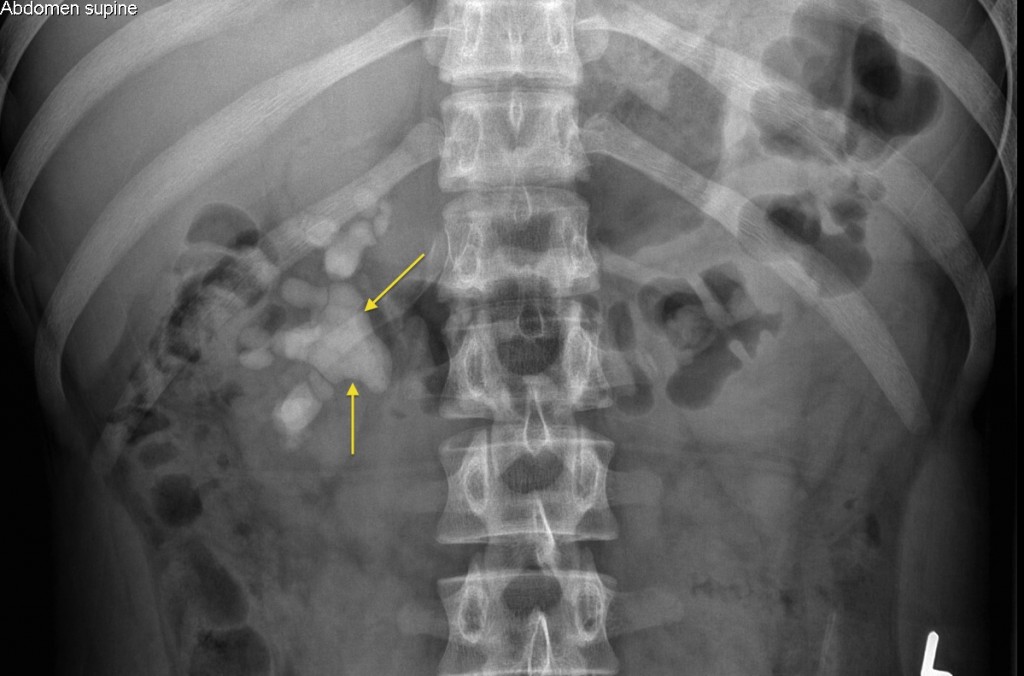
Over time, staghorn calculi often cause loss of renal parenchyma and function and sometimes lead to potentially fatal sepsis. This alkaline urinary environment promotes the crystallization of struvite and formation of exopolysaccharide biofilm with incorporation of microproteins into its matrix, becoming a nidus for repeated urine infections. Staghorn calculi are most frequently composed of mixtures of magnesium ammonium phosphate (struvite) and calcium carbonate apatite they are strongly associated with UTIs caused by organisms that produce the enzyme urease, which promotes the generation of ammonia and hydroxide from urea. A staghorn calculus is any stone that branches into more than one part of the collecting system. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
